Bladder leakage is one of the most common healthcare issues affecting women, with the effects of the condition having major effects on women’s lives. 1 in 3 women over the age of 18 experience bladder leakage at some point in their lives,1 and in general, prevalence increases at the start of the menopause. It is a major taboo and due to embarrassment women sometimes struggle to discuss the condition and need help.
It is now time for community pharmacy teams to take the lead and provide the proactive support your customers need – and don’t just reach for the pads... You can help them stop the leaks, and build customer loyalty. If women are regularly buying pads, or have struggled with using pharmacological solutions you can now offer alternative approaches.
What is incontinence?
Urinary incontinence is when a person accidentally passes urine when they don’t want to. It occurs when their bladder is put under pressure, such as when they cough, sneeze, laugh or run. Frequent or occasional, it can vary from a few dribbles to a complete loss of bladder control.
There are several known types of bladder and urinary incontinence. They receive their name from the origin of the issue that causes the passing of urine. Although they are similar and can have some of the same symptoms, they mostly differ in the way they come about:
Stress urinary incontinence (SUI) – causes the leak after a person strains or exerts themselves during a physical activity, including coughing, sneezing, laughing, running or jumping. This is the most common type of urinary incontinence.
Urge urinary incontinence (UUI) – if a person drinks a lot of fluid, or due to a range of physical causes, the a person can have a sudden urge to have to urinate. The leakage can vary from small drops to emptying the entire bladder.
Mixed urinary incontinence (MUI) – as the name suggests, it is a combination of SUI and UUI.
Overactive bladder (OAB) – simply means that a person needs to pass urine very frequently in a day, which can also come about suddenly such as UUI. Overactive bladder is a different issue and is best treated with prescription pharmacological drugs.
There are also neurological causes of bladder or urinary incontinence, such as damage of the nerves in the spinal cord (e.g., in neurological diseases - Parkinsons), or when a person cannot reach a toilet on time (called functional incontinence).
SUI is the most common type of incontinence affecting about 50% of women who experience UI.
What are the causes, and risk factors ?- Bladder leakage can affect women from an early age. Although the prevalence of bladder leakage increases with age, some women suffer from early on in life. In these cases, bladder leakage could be caused by an over-tight pelvic floor, due to frequent strenuous exercise.2
Pregnancy, childbirth and the menopause increase the prevalence of bladder leakage. These are the big three triggers. During pregnancy hormonal changes can cause the pelvic floor to relax, at a time when a growing baby is placing a lot of stress on those very muscles. Childbirth can then have a further weakening effect. Falling levels of oestrogen in peri- and post-menopausal women can reduce tissue plumpness and elasticity. This also weakens the pelvic floor muscles. All these factors increase the likelihood of experiencing bladder leaks.3
Physical activity – strenuous exercise, especially if performed frequently can cause on the pelvic floor muscle pressure over-tightness of the pelvic floor muscles which result in increased leaks.2
It is important to explain to women bladder leakage, caused by SUI, in majority of women is a mechanical issue, when the bladder angle needs correcting and bladder mobility limiting, and hence why drug treatment is not appropriate. In pharmacy, you should now see a minority of women presenting with prescriptions for SUI and UUI and medications used for incontinence are characterised by high levels of side effects and therefore low levels of compliance.
What treatments are available for bladder leakage in pharmacy and from the GP
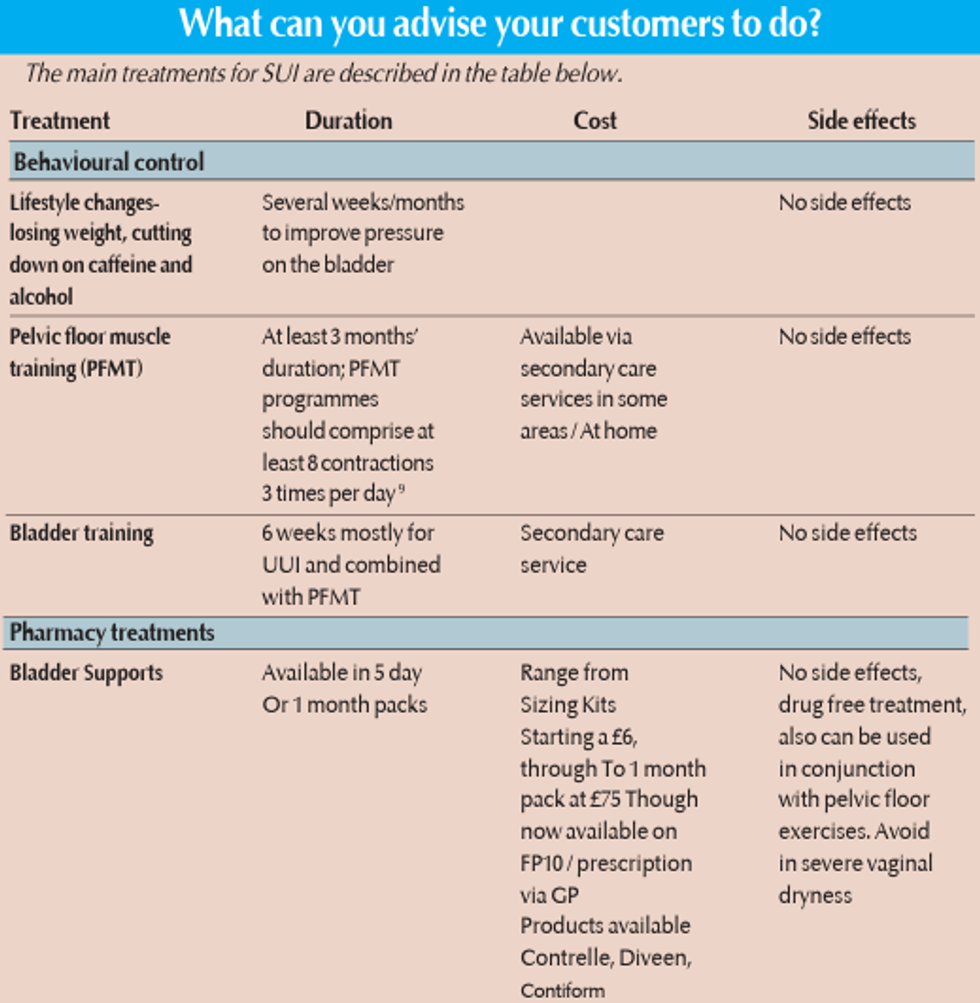
Several types of treatments are available for UI in women. These include: behavioural factors, non-surgical treatments, pharmacological treatments, and surgical treatments. These are used depending on the severity of the condition, which is included also described in the updated NICE Clinical guidelines [NG210].7,8, 10 Women will want your advice as majority of women want to treat the condition themselves, want immediate results, and see surgery as last resort.
Behavioural control approaches are the initial recommended approach, and recommendation to do pelvic floor exercises is key part of this initial approach. However, as most women will confide, it's not so easy. Recommend women to download the low cost NHS approved 'Squeezy' App to help them with their exercises, though many women struggle to do their pelvic floor exercises, because they do not have the coordinated function of pelvic floor muscles (PFM).
The PFM exercise is dependent on a complex neuro control consisting of voluntary muscle actions and reflexes, and it surprisingly common that many women do not have this connection so need your help.
It is important to discourage (STOP!) women using tampons for incontinence related symptoms, as such use can lead to drying of the vaginal mucosa and an increased risk of toxic shock.
Behavioural options will only work for some women and additional help in the pharmacy will be essential. Women have often resigned themselves to thinking no treatments are available and have just deferred to buying incontinence pads, unaware new innovation is now available.
Vaginal bladder supports are now available in pharmacy, and available on FP10, so a new approach to treatment is available for pharmacy teams with proven clinical results. For some women they will provide immediate benefits. The new UK NICE guideline now recommends the use of these vaginal devices as part of conservative therapy approach, and can used both when there is weakness in the pelvic muscle, and also where the muscle is too tight, which also can lead to leakage.
Bladder supports vary dependent on the materials they are made from, with women who want to exercise preferring products made from biocompatible soft foam.
Increasingly GP are recommending low-dose vaginal oestrogen therapy is a safe and effective option to treat menopause related symptoms or symptoms associated with UUI and SUI. These products can now also be sold over the counter from pharmacy. Reinforce to your patients these products are synergist in also benefiting the pelvic floor muscle structure, though remind them to continue to use as they take up to 12 weeks to have maximum effect, and need to be used for the long term.
Recommending and supporting your customers in using bladder supports
Bladder supports can provide your customers with immediate results and rapidly allow them to resume exercise and improve their quality of life. They need to find their correct size first – all brands have a sizing kit to start with and customers can do this themselves at home. When they have found their correct size then they can either purchase the required size or get on prescription from their GP.
Bladder supports are an ideal product for pharmacy recommendation as they can provide immediate results as they address the underlying mechanical need of supporting the bladder, immediately on insertion. Now pharmacy has the chance to recommend the solution to the problem and convert women from pads. All major bladder support brands are only available on prescription or via pharmacy ensuring high level of patient loyalty.
BY ANDREW TASKER
Andrew Tasker is Managing Director of Viveca Biomed.
References
- Hunskaar S, Lose G, Sykes D, Voss S. BJU Int.2004 Feb,93(3):324- 30
- (2022a). 10 ways to stop leaks how to help a weak bladder - NHS (www.nhs.uk)
- NHS (2022b). Urinary incontinence. Urinary incontinence - NHS (www.nhs.uk)
- Psychiatric aspects of female incontinence, International Urogynaecology Journal (2):69- 72
- Nygaard I, Delancey JO, Arnsdoff L. Exercise and incontinence Obstet Gynecol 1990;75:848-51
- Nilsson M, Lalos A, Lalos O. The impact of female Urinary incontinence and urgency on quality of life and partner relationship. Neurouol Urodyn 2009;28:976-81
- NICE guidance. (2015). Urinary incontinence in women: management. [NG171]. https://www.nice.org.uk/guidance/cg171
- NICE guidance. (2019). Urinary incontinence and pelvic organ prolapse in women: management. [NG123]. https://www.nice.org.uk/guidance/ng123
- (2019). Non-surgical treatment-Urinary incontinence. https://www.nhs.uk/conditions/urinary-incontinence/treatment/
- NICE guidance. (2021). Pelvic floor dysfunction: prevention and non-surgical management. [NG210]. https://www.nice.org.uk/guidance/ng210