Key Summary
- From September, immunosuppressed adults aged 18–49 will be eligible for the Shingrix jab
- JCVI found younger high-risk groups face similar hospitalisation risks as older patients
- Vaccination cuts severe illness, with thousands of cases and complications already prevented since 2013
NHS has decided to increase its shingles vaccination cover by including immunosuppressed adults between 18 and 49 years from September.
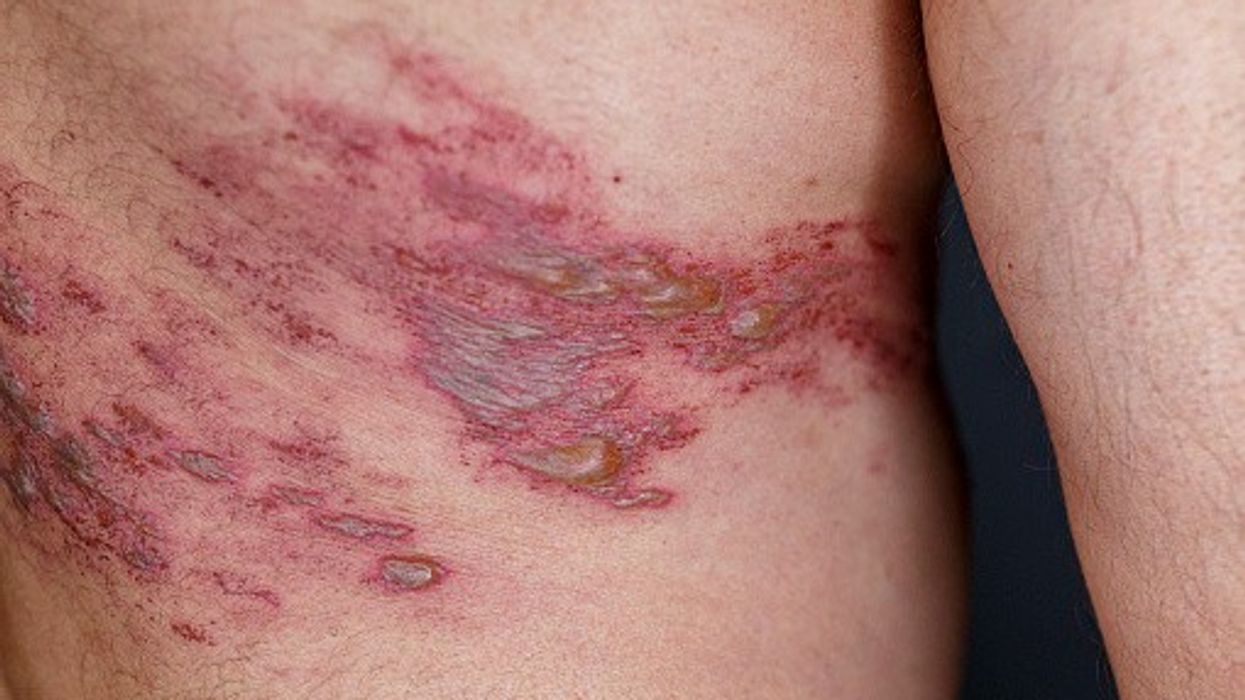
Shingles is caused by the reactivation of the varicella zoster virus (which causes chickenpox) and usually occurs decades after initial infection.
People with severely weakened immune system, or suffering from leukemia, lymphoma, and those who undergo chemotherapy are eligible.
Those eligible can book their appointments via their GP surgery for Shingrix vaccine.
This change in eligibility criteria was recommended by Joint Committee on Vaccination and Immunisation (JCVI), which found that the risk of hospitalisation from shingles or those resulting in post-herpetic neuralgia was similar in younger immunosuppressed age groups to those who were already eligible.
This vaccine is currently being given to people from 65 to 79 years of age, and severely immunosuppressed people in their 50s.
“Following a review of the evidence, it was found that younger adults who are severely immunosuppressed are also at higher risk of severe illness and hospitalisation,” said Dr Gayatri Amirthalingam, deputy director of immunization at the UK Health Security Agency.
Those afflicted by shingles develop painful rashes that lasts 2–4 weeks.
It can by treated completely, but it could leave the patients with persistent pain known as post-herpetic neuralgia, eye problems, pneumonia, hepatitis, brain inflammation, etc.
The JCVI also found that before the shingles vaccination programme began in 2013, over 4,500 people were hospitalised each year, most cases preventable with vaccination.
Within the first 3 years of the vaccination programme, there were an estimated 17,000 fewer episodes of shingles and 3,300 fewer episodes of post-herpetic neuralgia among the eligible population.
“The vaccine is safe and effective and significantly reduces the chance of developing shingles and becoming seriously unwell, so I’d urge anyone newly eligible to come forward for their protection as soon as possible,” said Dr Amanda Doyle, national director for primary care and community services at NHS England.