Achieving the community pharmacy vision necessitates legal adjustments and additional funding beyond recent boosts, the pharmacy vision document published by Nuffield Trust and The King's Fund has revealed. It says community pharmacies in England must adapt to changing population needs amidst unprecedented health and care challenges.
Commissioned by Community Pharmacy England, the report titled 'A Vision for Community Pharmacy', published on Sept. 19, is a result of almost a year of research and extensive consultation with the sector and wider stakeholders, advocating for community pharmacy. The think tanks detail a shift in the community pharmacy sector, highlighting how pharmacies can contribute to crucial policy objectives regarding population health, prevention, and the increasing demand in primary care.
"The health and care needs of the population are evolving, and pharmacies in England, like all components of the health and care system, must adjust to address these changes," said Helen Buckingham, Director of Strategy at Nuffield Trust.
"Community pharmacies hold a crucial and promising role in assisting patients in leading healthy lives, accessing prompt and effective treatments, and navigating their healthcare,” she added. “While many pharmacies are already engaged in this effort, barriers at both national and local levels hinder them from realizing their full potential. This vision for community pharmacy outlines the substantial transformation anticipated in the pharmacy landscape over the next decade."
The report analysed previous barriers and delineated necessary steps for surmounting them, highlighting vital factors that strengthen confidence in the sector's current progress towards realising the vision.
"Despite ongoing pressure on our healthcare services, this vision presents an opportunity to invest in the future by harnessing the experience and expertise within community pharmacies," said Richard Murray, Chief Executive of The King’s Fund. "Broadening their scope would enable pharmacies to keep more individuals in good health. For instance, this could involve aiding them in managing common long-term conditions, reducing the necessity for frequent GP visits, or extending their capabilities to diagnose and treat a wider array of minor conditions."
“This independent vision for community pharmacy lands at a pivotal moment as we look to conclude negotiations on the £645 million investment in community pharmacy and prepare for discussions on what comes after April 2024,” said Janet Morrison, Chief Executive of Community Pharmacy England. “With community pharmacies in crisis, the sector needs to influence more effectively than ever before and working with a wide range of partners who also have influence in Government and the NHS – like these two leading think tanks – is an absolute must,” she added.
Enhancing pharmacy empowerment
The King’s Fund and Nuffield Trust suggest enabling pharmacists to directly refer patients for scans, blood tests, and to hospitals and specialists when necessary. This complements the initiative to increase the number of pharmacists qualified to prescribe medicines and treatments by 2026.
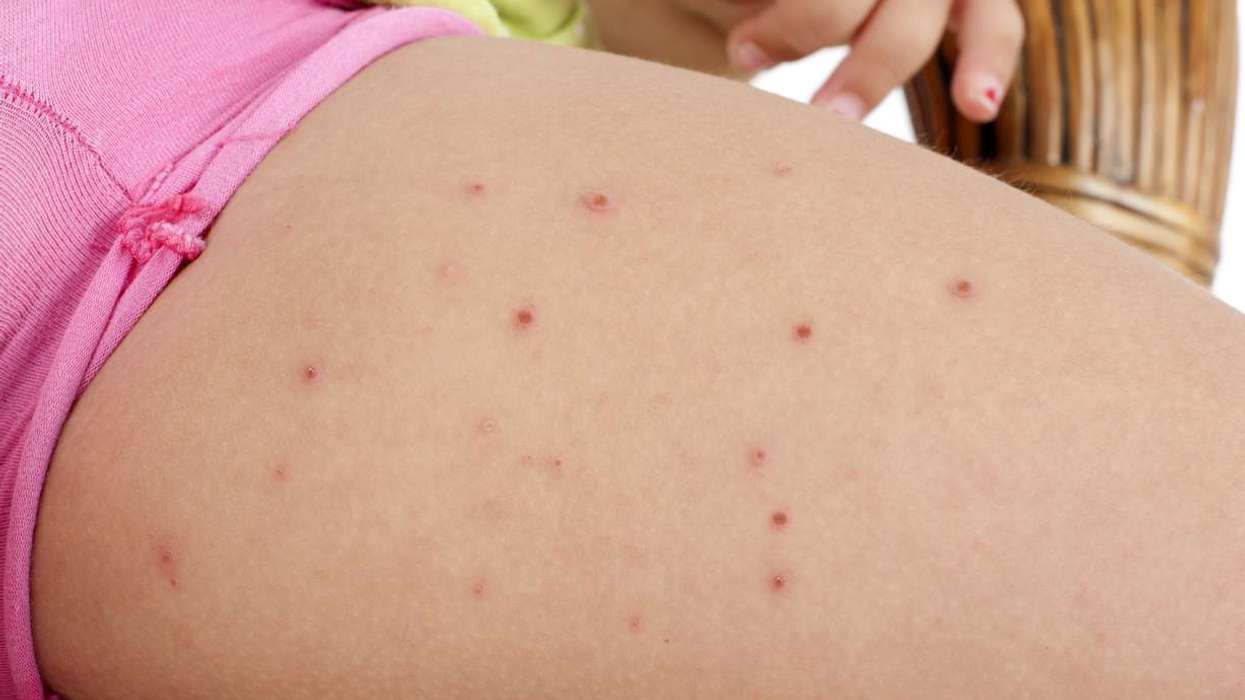
According to the think tanks, certain community pharmacists presently address minor conditions and provide contraception services. Yet, with the realisation of this vision, this service scope would broaden. Pharmacies across England would be equipped to diagnose and manage conditions like chickenpox and UTIs. This means a significant share of patients with minor or manageable illnesses would receive treatment from a pharmacist.
However, the report identifies persistent obstacles in realizing this vision, stemming from outdated infrastructure, equipment, and IT systems, as well as challenges in staff training, regulation, and integrating pharmacies with other primary care services.
The key barriers include:
- A lack of investment in buildings, digital infrastructure and staffing across primary care, with new models of care reliant on shifting resources from one part to another rather than increasing overall investment.
- Complex finance and contracting arrangements that inhibit new models of pharmacy, with hard-to-manage and fragmented contracts and perverse incentives which block a shift away from dispensing.
- Insufficient management capacity and capability within community pharmacy and within developing integrated care boards.
- Poorly developed local relationships between professionals which inhibit integration and create some mistrust between primary care professionals.
- A lack of patient data and access between primary care professionals of patient records.
- The public and patients still think of pharmacy as limited to the dispensing of medicines and retail.
Meanwhile, the report makes a series of recommendations for national bodies and policymakers, which include:
- Greater investment in IT and data to ensure that any pharmacies who offer enhanced services have access to the National Care Records Service and additionally to ICB-level shared care records to allow better data sharing.
- In the coming years, pharmacy funding to cover this expanded role will need to rise above the £645 million for extra services recently committed to by NHS England over two years.
- Legislative changes to contract rules to allow dispensing without a pharmacist on site, in order to free up pharmacists to make the best use of their skills and systems that allow safe and accurate dispensing in this scenario.
- Consideration of incentives that would make it easier for pharmacists to put the necessary time and effort into closer collaboration with other local primary care services, including payments to free up pharmacy and GP time when working together on local issues, coupled with investment to build up capacity rather than moving it around the sector.
- ICBs need sufficient resource and time to deliver oversight and support to the community pharmacy sector and where appropriate build in external support for smaller independent pharmacies.
- The NHS contract for the delivery of community pharmacy services will need to be revisited to deliver this vision, alongside agreement at national level about how community pharmacy fits within the broader primary care strategy.
- An information campaign at both national and local levels to ensure that patients and the public are aware of the services available in local pharmacies and how to access them.
Envisioning pharmacies of tomorrow
Nuffield Trust and The King’s Fund depict pharmacies of the future as dynamic enterprises, upholding their pivotal role in the medicines supply chain, and broadening the scope of contracted and funded services they offer. Pharmacy teams will leverage their professional expertise, forging even closer collaborations with colleagues within local healthcare networks, the study noted.
The think tanks identified a range of actions necessary to achieve their vision, with a sustainable funding package and active engagement with other parts of the health service at the forefront of their strategy.
"Some pharmacies may find this vision not bold enough, while for others, achieving the outlined services might seem like a pipedream," Morrison added. "Many of you will rightly question whether the barriers and obstacles identified by Nuffield Trust and The King’s Fund can be overcome. However, in this vision, the think tanks have aimed to encompass the entire range of pharmacy perspectives, presenting the sector as the solution it truly is, while also outlining the necessary steps for pharmacies to flourish. Having independent experts set such a clear direction will be a potent tool for us."
Morrison said that CPE supports the direction of travel that has been set out in the report and hope the sector will come behind this.
"The blueprint will prompt policymakers to envision a different future for pharmacies and guide us in turning that vision into reality," she said. "It supports our objectives in highlighting to current and future governments, as well as the NHS, the extensive contributions made by pharmacies. It demonstrates the significant challenges you face, forewarns of potential repercussions if support is lacking, and offers viable solutions that they would be inclined to invest in."
Morrison emphasised that realising aspects of this vision and securing the future of pharmacy will necessitate concerted efforts from both local and national NHS commissioners, as well as the government, and everyone involved in community pharmacy.
Imperative measures
CPE intends to incorporate the report's recommendations into its strategic efforts to enhance the future trajectory of community pharmacy. This becomes especially pivotal as negotiations for the Community Pharmacy Contractual Framework (CPCF) loom following the conclusion of the five-year deal.
According to CPE, the development of such a strategy aligns with a key recommendation from the Pharmacy Representation Review Steering Group (RSG). 'The Vision will be particularly instrumental in kick-starting crucial policy dialogues with both national and local commissioners. With the backing of LPCs, we aim to collaborate with national and local healthcare systems to advance this initiative,' states CPE."
"The Vision has already garnered parliamentary attention, being referenced in a debate last week. Today, we are hosting a reception for the Vision in Parliament, which will be attended by MPs, NHS policy leaders, health charities, and patient representatives," Morrison stated. "This advocacy work will persist, featuring events at political party conferences and a succession of policy roundtables with pertinent stakeholders. Additionally, we will assist LPCs in engaging with leaders of Integrated Care Systems (ICS)."
Morrison emphasised that actively involving the Government, the NHS, and broader stakeholders in advancing aspects of the Vision will be a central focus of CPE’s advocacy efforts in the upcoming months. The hashtag #PharmaciesOfTomorrow will be employed to underscore this initiative, she added.
On September 14, a parliamentary debate centred on the future of community pharmacies addressed crucial topics such as financial strains, workforce shortages, and pharmacy closures. The discussion delved into the pressing challenges confronting pharmacies, with the aim of formulating concrete solutions for a sustainable future in the sector."
"For this vision to be realised, it will require determination and commitment not only from the NHS but also from the community pharmacy sector itself," added Murray of The King’s Fund. "If the community pharmacy steps up to seize these new opportunities, there will be benefits to their business, and critically, they can provide better and more convenient access to health services for patients and the public."
RPS England embraces the vision document
Today's report is a valuable contribution to this discourse, offering a clear roadmap for the Government and the NHS to optimise the role of community pharmacy in enhancing patient care, RPS England said.
"Through our collaboration with The King’s Fund last year, health and care leaders consistently emphasised the integral role of community pharmacy in shaping the future of healthcare," said Tase Oputu, Chair of RPS England.
Oputu said that there are some key enablers to make this a success, including workforce planning to ensure a pipeline of pharmacists for the future, making best use of skill mix within pharmacy teams, and much-needed investment in IT and interoperable patient records.
“It is vital that pharmacist and pharmacy teams are now supported across the system to help make the most of community pharmacy’s potential, delivering more integrated care and developing new services to reduce health inequalities and continue making a difference for patients,” she added.