Many of us in community pharmacy are used to dealing with a patient presenting with acute eye problems. With the Quality Pharmacy Scheme also now seeing pharmacist having conversations with diabetic patients about their eye care, the importance and role of community pharmacy in helping people maintain good eye health is becoming more prominent.
Let’s look at some common eye complaints:
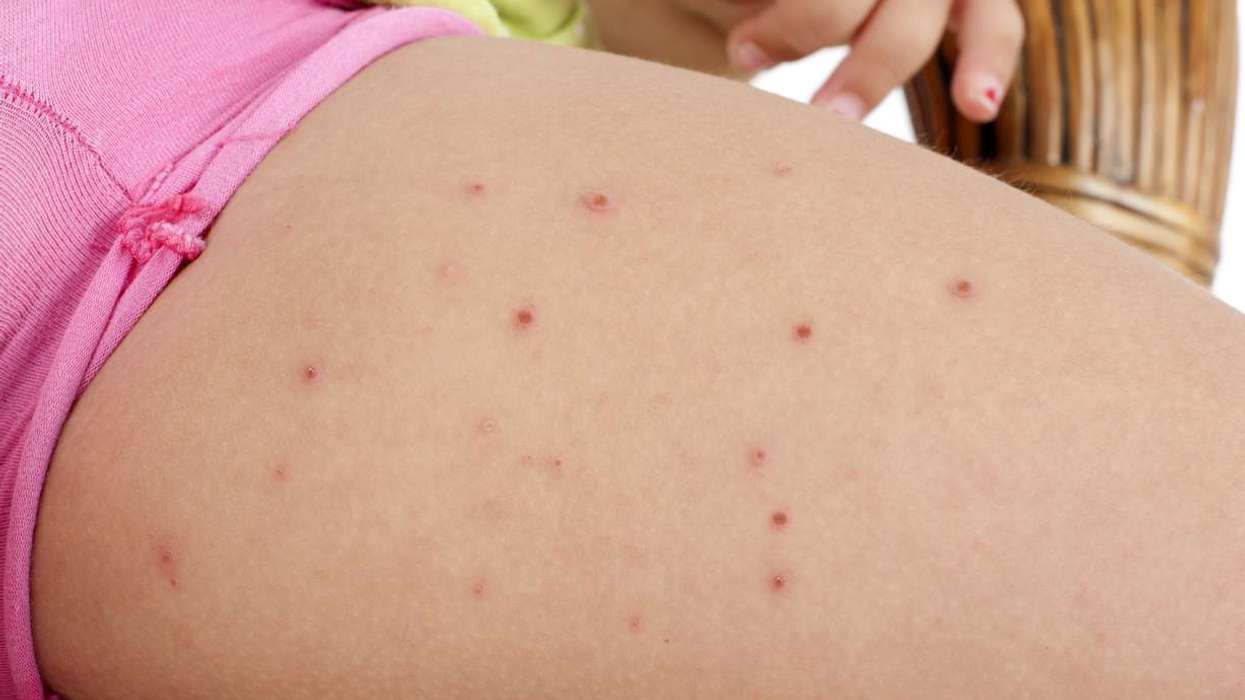
Conjunctivitis, commonly known as red-eye or pink-eye, is inflammation of the conjunctiva, the thin tissue layer that covers the eye. It can be allergic or infective in origin and treatment should vary accordingly.
Allergic conjunctivitis usually presents itself with watery discharge, oedema, itching and is commonly bilateral. Patients may also be suffering from systemic symptoms such as rhinitis, runny nose.
Patients should be advised to avoid allergen wherever possible. Hayfever and pet allergies are very common. Some patients may benefit from wearing wraparound sunglasses throughout the hay fever season.
Topical mast cell stabilisers, such as sodium cromoglycate, may be used as a prophylactic treatment and work by inhibiting the release of inflammatory mediators. The drops must be used regularly to achieve the therapeutic benefit, and it may take up to 14 days to work and their use should be continued while the patient is exposed to the allergen.
Another suitable treatment option is antihistamine/ decongestant eye drop combination such as Otrivine though they are recommended for short-term use no more than consecutive seven days, as prolonged use may cause rebound effects.
Infective conjunctivitis can be viral or bacterial. Bacterials present with yellow, purulent discharge and typically begin in one eye before spreading to the other, whereas viral presents bilaterally with a watery discharge and often is associated with URTI symptoms. Both bacterial and viral conjunctivitis are associated with a gritty feeling within the eye.
It is essential to differentiate this from actual pain as this can be indicative of something more severe and should be referred. Other referral points are any changes in vision, photophobia, clouding of the cornea and any recent trauma (whether chemical, mechanical or blunt trauma).
Ocular antibiotics are beneficial for treating bacterial infections though they are usually self-limiting and should resolve themselves within two to five days. Currently, the first-line treatment in the UK is chloramphenicol drops or ointment, which is obtainable over the counter for anyone over two years.
Patients should be reminded that infective conjunctivitis is very contagious, and measures should be taken to avoid spreading the infection, such as not sharing pillows and towels and washing hands thoroughly after touching the eye area.
Contact lenses should not be worn when there are signs of infection and should be avoided until all signs of infection are gone. Where drops are used, patients using soft contact lenses should stop their use throughout treatment and for 48 hours afterwards as some preservatives in the drops can damage the lenses.
There is currently no specific OTC treatment for viral conjunctivitis. Patients should be reassured that it usually is self-limiting and should resolve within one to two weeks. Management techniques include cool compresses applied tenderly around the eye area and the use of lubricating drops (such as hypromellose) to aid comfort and removing any discharge by cleaning the eyelids with cotton wool soaked in boiled and cooled water.
Dry eye management
Dry eye is a deficiency of the conjunctival mucous or a tear deficiency which can lead to irritated eyes with varying levels of discomfort. It can be associated with older age and is often worsened by environmental factors such as dry air, wind, dust and smoke.
As we all spend more time staring at digital screens, this is also contributing to making it more common. Staring at a computer screen, phone or other handheld devices these days can cause strain the eyes significantly. A decrease in tear production can be a result of an adverse drug reaction. Such drugs include diuretics, oestrogen, beta-blockers and antimuscarinics (e.g. antihistamines and tricyclic antidepressants). Though they may be managed over-the-counter in the meantime, suspected ADR’s should be referred back to the prescriber. Other referral points include diabetes and previous trauma.
Management should include attempts to avoid any causative factors and treatment with ocular lubricants such as Hypromellose or carbomer 980 gel. In those needing frequent applications, it may also be worth considering an ointment over a drop as those are more viscous and adhere to the eye for an extended period.
It is worth noting that preservatives in ocular preparations may cause a local inflammatory response, in this case, it may be worth considering a preservative-free formulation. A preservative-free formulation should also be considered in those patients whose symptoms require application more than six times daily as this may overcome irritation.
Patients should be reminded to upkeep regular opticians’ visits. It is generally recommended that our eyes are checked every two years unless otherwise advised by an optometrist.
An eye examination not only detects changes in vision but can also help to discover underlying health conditions and may help with early diagnosis of eye problems, thus enabling earlier treatment.
Patients should be reminded about protecting their eyes from the sun, the use of UV resistant sunglasses should be recommended. Patients should also be told to never look directly at the sun as this can cause permanent damage.
Advice for patients
At Bedminster pharmacy, we always advise all our patients and carers on the use and storage of all ophthalmic preparations. We also give talks in local residential and sheltered accommodations to help.
After using an eye ointment, patients may find that their vision is temporarily blurred though this should be cleared by blinking. Following the use of eye drops patients should be advised to hold the inner corner of the eye (closest to the nose) for a minute, this reduces systemic absorption and can stop the bitter taste some patients experience with eye drop application.
When a patient is required to take several drops, generally, the order in which this is done is insignificant so long as there is a gap of around five minutes between each administration to allow for absorption. Though it is favourable that ocular lubricants are applied last so that they are not washed away by other ocular preparations.
This article also appears in the February issue of Pharmacy Business.